HÖRST
outer ear infection


Table of contents
An outer ear infection, also known as otitis externa, is an inflammation of the external ear canal that can occur for various reasons. This condition affects both adults and children and is particularly common in the summer months when many people spend more time in the water. Otitis externa is often referred to as "swimmer's ear" because it frequently occurs after prolonged contact with water. In this comprehensive guide, you will learn everything about the causes, symptoms, diagnosis, and treatment of this painful condition.
What exactly is an outer ear infection?
Otitis externa is an infection or inflammation of the external auditory canal, which extends from the outer ear to the eardrum. This condition is painful and can significantly interfere with daily life. The risk of developing otitis externa increases when the ear canal remains moist, for example after swimming or showering. However, the condition can also be caused by mechanical irritation, such as inserting foreign objects or cotton swabs into the ear canal.
Otitis externa differs from otitis media, which affects the middle ear and is more common in young children. While otitis media is caused by colds and upper respiratory tract infections, otitis externa is often caused by external factors.
- Bacterial infections: The majority of outer ear infections are caused by bacteria, particularly Pseudomonas aeruginosa and Staphylococcus aureus. These bacteria can enter the ear canal, especially if the natural protective layer of the ear canal skin is weakened. This often happens when the ear canal is moist, for example after swimming.
- Fungal infections: In some cases, otitis externa can be caused by fungi, especially in tropical or humid climates. Fungal infections of the ear canal are less common but can be particularly stubborn and require longer treatment.
- Injuries to the skin of the ear canal: Inserting foreign objects such as cotton swabs or hairpins into the ear canal can injure the skin of the ear canal and lead to inflammation. These micro-injuries provide an ideal breeding ground for bacteria and fungi to multiply and cause infection.
- Skin conditions: Certain skin conditions, such as eczema or psoriasis, can make the skin in the ear canal more susceptible to infection. These conditions irritate and inflame the skin in the ear canal, increasing the risk of outer ear infection.
- Earwax and irritants: Earwax plays an important role in protecting the ear canal by keeping out dirt and bacteria. However, excessive or improper removal of earwax can damage the natural protective layer of the ear canal skin and cause inflammation. In addition, chemical irritants such as certain shampoos or hair dyes can irritate the ear canal and trigger otitis externa.
Recognizing symptoms of an outer ear infection
The symptoms of otitis externa can vary greatly depending on the severity of the inflammation and the underlying cause. The most common signs of an outer ear infection include:
- Earache: Earache is the most common symptom of an outer ear infection. The pain can range from mild to very severe and is often made worse by touching or moving the ear. The pain can also radiate to the jaw or throat and be particularly intense when chewing.
- Itching in the ear canal: Persistent itching in the ear canal is a common early symptom of an outer ear infection. Scratching can aggravate the inflammation and should be avoided.
- Discharge from the ear: Severe inflammation can cause yellowish or greenish discharge from the ear. This discharge usually consists of pus and indicates a bacterial infection.
- Feeling of congestion in the ear: Many affected individuals report a feeling of pressure or congestion in the ear. This can be caused by swelling in the ear canal or by the build-up of pus.
- Temporary hearing loss: If the ear canal is severely inflamed or blocked by pus, this can lead to temporary hearing loss. This usually disappears after the inflammation has been treated.
- Swelling and redness of the ear: In some cases, the outer ear, including the ear lobe, may be swollen and red. This is a sign that the inflammation has spread to the surrounding tissue.
Diagnosis of an outer ear infection
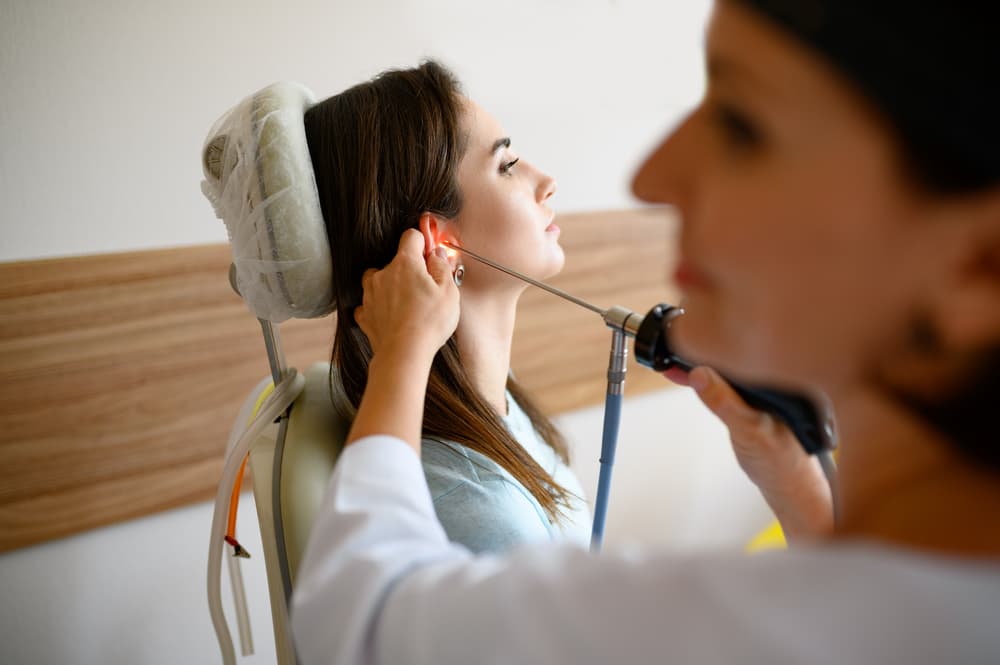
An outer ear infection is usually diagnosed through a clinical examination. The doctor will examine the ear with an otoscope, a special instrument that allows them to view the ear canal and eardrum. During the examination, the doctor can see whether the ear canal is swollen or inflamed and whether there is any pus or other fluid present.
In some cases, the doctor may take a sample of the discharge to identify the specific bacteria or fungi that caused the infection. This is particularly important if the infection does not respond to standard treatment or is recurrent.
Treatment options for outer ear infections
The treatment of an outer ear infection depends on the severity of the inflammation and the underlying cause. In most cases, a combination of medication and self-care is recommended.
- Medication: The most common treatment for bacterial outer ear infections is antibiotic ear drops. These drops are applied directly into the ear canal to fight the bacteria and relieve the inflammation. Antibiotics are particularly effective for bacterial infections and are often prescribed together with corticosteroid drops to reduce swelling and itching.
Antifungal ear drops are used to treat fungal infections. These can be used for several weeks to ensure that the fungal infection clears up completely. - Pain management: Pain relievers such as ibuprofen or acetaminophen can be taken to alleviate pain. These medications also help reduce inflammation and improve overall well-being.
- Cleaning the ear canal: In some cases, it may be necessary to have the ear canal professionally cleaned by a doctor, especially if pus, dead skin cells, or excess earwax has accumulated. This can be done by gently suctioning or rinsing the ear canal.
- Avoiding water in the ear: During treatment, it is important to keep the ear dry to prevent the inflammation from worsening. This can be achieved by wearing earplugs when showering or bathing.

Preventive measures against outer ear infections
Preventing otitis externa is particularly important in order to avoid recurring infections. Here are some tips on how you can reduce the risk of outer ear infections:
- Keep your ears dry: After swimming or bathing, make sure your ears are completely dry. Tilt your head to the side to allow water to drain from the ear canal and use a soft towel to gently dry the ear. Carefully removing excess earwax can also help reduce the risk of inflammation.
- Do not insert foreign objects into the ear canal: Avoid inserting cotton swabs, fingers, or other objects into the ear canal. These can damage the sensitive skin of the ear canal and cause inflammation.
- Protection when swimming: If you swim frequently, you should consider using special earplugs to prevent water from entering the ear canal. These are available at pharmacies and can significantly reduce the risk of otitis externa.
- Treat skin conditions: If you suffer from skin conditions such as eczema or psoriasis, you should treat them specifically to minimize the risk of outer ear infection. Your doctor can prescribe special creams or ointments that protect and care for the skin in the ear canal.
- Be careful when using hearing aids and headphones: Hearing aids and in-ear headphones can increase the risk of outer ear infections if they are not cleaned regularly. Be sure to keep your devices clean and disinfect them regularly to prevent infections.
Long-term consequences and complications of an outer ear infection
Although most outer ear infections respond well to treatment and resolve without long-term consequences, complications can occur in some cases, especially if the condition is not treated properly.
Chronic otitis externa
Untreated or inadequately treated outer ear infections can become chronic. In this case, recurrent inflammation occurs, which can impair hearing and lead to permanent damage to the ear canal.
perichondritis
In severe cases, the inflammation can spread to the ear cartilage and the outer ear, causing a condition known as perichondritis. This condition is difficult to treat and can lead to permanent deformation of the ear.
Spread of infection
In rare cases, the infection can spread to the surrounding tissue or even to the middle ear, which can lead to middle ear infection or mastoiditis. These complications require more intensive treatment and can have serious consequences.
When should you see a doctor?
It is important to take the symptoms of otitis externa seriously and consult a doctor if necessary. You should seek medical attention if:
- The pain does not subside or worsens despite the use of painkillers.
- You notice sudden or persistent hearing loss.
- You develop a fever, which could indicate a more serious infection.
- Purulent or bloody discharge from the ear
Seeing a doctor early on can help prevent complications and speed up healing.
Further articles

Healthy candy alternatives for seniors

Cooking together in old age
